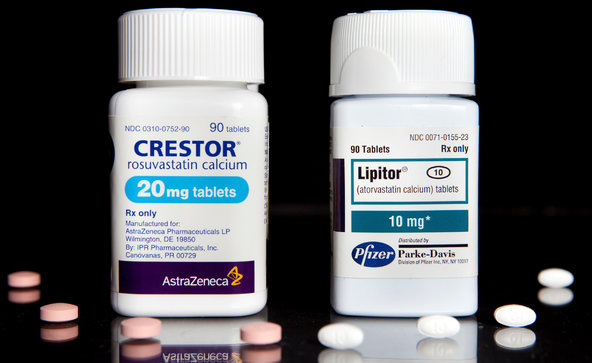
“Statin Drugs stimulate atherosclerosis and heart failure” is the title of a research study published recently that has been turning many heads in the clinical world. It has not made mainstream news at the time of this article writing, but it is of utmost importance to the health of the tens of millions taking statin drugs for cholesterol. The evidence continues to pile up and prove that statin drugs are hazardous to your heart and health.
The study, published in Expert Review of Clinical Pharmacology February 6, 2015, discusses the process of how statin drugs cause the demise of heart health, worsen atherosclerosis and induce heart failure. The study’s authors are located in Japan at the Nagoya City University. If and when this news reaches the American public, the tens of millions of patients on statin drugs with worsening heart disease and heart failure should be flooding their physician’s office and the drug companies’ door with phone calls demanding explanations and reprimand. So far that has not happened.
Here is the Abstract from that research:
In contrast to the current belief that cholesterol reduction with statins decreases atherosclerosis, we present a perspective that statins may be causative in coronary artery calcification and can function as mitochondrial toxins that impair muscle function in the heart and blood vessels through the depletion of coenzyme Q10 and ‘heme A’, and thereby ATP generation. Statins inhibit the synthesis of vitamin K2, the cofactor for matrix Gla-protein activation, which in turn protects arteries from calcification. Statins inhibit the biosynthesis of selenium containing proteins, one of which is glutathione peroxidase serving to suppress peroxidative stress. An impairment of selenoprotein biosynthesis may be a factor in congestive heart failure, reminiscent of the dilated cardiomyopathies seen with selenium deficiency. Thus, the epidemic of heart failure and atherosclerosis that plagues the modern world may paradoxically be aggravated by the pervasive use of statin drugs. We propose that current statin treatment guidelines be critically reevaluated.
Vitamin K2
The study presented insightful information describing the physiological mechanisms on how statin drugs cause coronary artery calcification or stiffening of blood vessels perpetuating the atherosclerosis. The plaque build-up occurs because statin drugs inhibit vitamin K2 function in the body. Vitamin K2 protects arteries from calcification. Without proper levels and function of vitamin K2, plaque levels worsen because of negative interaction with the Gla-protein and the inhibition of vitamin K2. This was previously described in a large study in 2012 with the same conclusion – statin use causes increased presence of coronary plaques. They did not identify the link with vitamin K2. The tool that cardiologists use to prevent atherosclerosis actually worsens it.
Mitochondria Damage
The second finding of the study is of little surprise. It shows that statin drugs are toxic to the mitochondria, or the energy producers in cells. Mitochondrial damage in the heart is a downward slope to cardiomyopathy or heart failure. This is a dangerous, although often subtle, effect. Statins impair the heart muscle mitochondria function, severely disrupt ATP production, and alter intracellular signaling proteins. This impairment leads to muscle cell dysfunction and eventually apoptosis or muscle cell death. This is like pouring concrete into the cellular engines of energy production and heart muscle contraction. Statins are notorious for depleting coenzyme Q10 out of the heart muscle and the body. This profoundly interferes with mitochondria function. Statins also interfere with the protein called heme A. Heme A is a component of hemoglobin that helps bind onto oxygen and carry iron to the muscle cells in the heart. Without the ability to transport iron and oxygen to the heart cells, energy production is further compromised. Iron deficits in the heart myoglobin may occur and possibly contribute further to heart failure.
Coenzyme Q10
Statin drugs interfere with coenzyme Q10. This has been documented repeatedly in medical literature with strong evidence. In fact, a black box warning for statin drugs or HMG CoQ reductase inhibitors was proposed to the FDA. The proposed black box warning was:
“HMG CoA reductase inhibitors block the endogenous biosynthesis of an essential co- factor, coenzyme Ql0, required for energy production. A deficiency of coenzyme Q10 is associated with impairment of myocardial function, with liver dysfunction and with myopathies (including cardiomyopathy and congestive heart failure). All patients taking HMG CoA reductase inhibitors should therefore be advised to take 100 to 200 mg per day of supplemental coenzyme Q10.”
The FDA blocked the attempt of putting a black box warning on statin drugs in 2014. How egregious is that?
Selenium
Another factor discussed in the initial study was the interference of the production of selenium containing proteins. Statin drugs inhibit the biosynthesis of these selenoproteins. One of the most important selenoproteins in the body is a compound called glutathione peroxidase. Its job is to protect the organism, especially muscle tissue, from oxidative damage coming from hydrogen and lipid peroxides. Lack of the glutathione peroxidase enzyme promotes high levels of free radical activity and tissue damage. Blocking the selenoprotein enzyme glutathione peroxidase is akin to pouring gasoline on the fire of inflammation and free radicals, which damages muscle tissue. In fact, the scientists described this blocking of the selenoproteins reminiscent of selenium deficiency induced heart failure, known as Keshan’s disease first identified in the 1930s. Scientists have strongly recommended that individuals suffering from non-ischemic heart failure have their selenium levels tested. This is a blood test that is readily available. Get an RBC selenium level checked at your next appointment. Certainly our selenium depleted foods and soils are not helping this situation when combined with drug-nutrient induced deficits.
Other Side Effects
 Expand this picture further. We have skeletal muscle, cardiac muscle, and smooth muscle. The side effects of statin drugs are often discussed as skeletal muscle weakness and pain and in recent years the increased development of heart failure (cardiac muscle failure). This is most often in the context of high dose statins. There are, however, other side effects that may be linked with statin drugs and how they affect mitochondria. Common side effects with the drug simvastatin include headaches and constipation. One doesn’t normally think of headaches and constipation concerns linked with mitochondria, but they can be. Both the nervous system and smooth muscles have high levels of mitochondria. Bowel motility is dependent upon smooth muscle function and nervous system activity. When there is a disruption in the health of mitochondria in the body, one of the symptoms may be constipation.
Expand this picture further. We have skeletal muscle, cardiac muscle, and smooth muscle. The side effects of statin drugs are often discussed as skeletal muscle weakness and pain and in recent years the increased development of heart failure (cardiac muscle failure). This is most often in the context of high dose statins. There are, however, other side effects that may be linked with statin drugs and how they affect mitochondria. Common side effects with the drug simvastatin include headaches and constipation. One doesn’t normally think of headaches and constipation concerns linked with mitochondria, but they can be. Both the nervous system and smooth muscles have high levels of mitochondria. Bowel motility is dependent upon smooth muscle function and nervous system activity. When there is a disruption in the health of mitochondria in the body, one of the symptoms may be constipation.
This is the same with migraines. Some types of headaches, i.e. some subtypes of migraines are related with mitochondria dysfunction. Joint pain and tendon problems may also be related. Don’t forget the brain and side effects of being forgetful or depressed. Our brain desperately needs healthy mitochondria to function effectively. It is common to dismiss these symptoms, attributing them to poor diet, stress, or aging. Yet, how many statin users have the common symptoms of constipation, headaches, joint pain, and feel a little less energetic, forgetful, and weaker than they did a few years ago and chalk it up to aging. Often they go to their physician and because they do not have outright symptoms of rhabdomyolysis and liver failure from the statin drug, it is chalked up to stress and getting older. The traditional medical and research communities are heavily debating these side effects and are not owning up to the real damage caused by statins. Many are looking for more ways to prescribe statins other than for cholesterol problems.
The question remains: how many people are going to suffer further heart disease with sky-rocketing rates of heart failure and subsequent loss of function and life linked with statin induced side effects? How many burgeoning statin drug class action law suits will it take to stop the pharmaceutical industry from this massive debacle and cover-up resulting in human tragedy? One is too many. It is time for the medical and pharmaceutical industry to acknowledge the truth and look at real solutions for heart disease.
Proactive Steps
If you are on statin drugs for any reason, make sure that you are taking at least 200 mg of coenzyme Q10 per day. Higher amounts, up to 600 – 800 mg, may be used for serious fatigue, mitochondrial injury, and cardiomyopathy disorders. The form of coenzyme Q10 plays a substantial role in how well coenzyme Q10 is absorbed, gets into the blood stream, and where it is used in the cell. Wellness Resources recommends the use of water and fat soluble coenzyme Q10 in either ubiquinone or ubiquinol forms.
Supporting selenium levels is also of primary concern. Brazil nuts, some seafood, mushrooms, asparagus, poultry and beef may provide good dietary sources of selenium or consider nutritional supplementation for standardized activated forms of selenium, like seleno-methionine.
Vitamin K2 must be present in adequate amounts to offset the drug-nutrient interaction. It is found in fermented foods and limited quantities in animal products. It is also produced by healthy gut bacteria and available in supplemental form.
Protecting the mitochondria from further oxidative damage should also be a priority. This is irrespective of statin drug use. Antioxidant rich, deep colored fruits and vegetables help protect the mitochondria from oxidative stress. Nutrients described above and others such as resveratrol, carnitine, bacopa monniera, curcumin, all B vitamins, vitamin C, vitamin E, K1, NAC, and lipoic acid are just some of the nutrients essential for protecting the heart from ischemic/heart attack damage, heart failure, and mitochondria injury.
Interestingly, in the last ten years melatonin has been found to protect the heart after heart attack injury in animal studies. Melatonin stopped heart cells from dying and protected the structural integrity of the mitochondria in heart cells and avoided marked worsening of heart damage. This too can be added to the arsenal of support for protecting the heart.
The link of melatonin and its ability to protect the heart and mitochondria leads into another tangent – the thought of sleep deprivation, sleep hygiene, and light exposure in the body and its effect on the body. With heart disease, heart failure and mitochondrial disorders at epidemic levels, it makes one question the age of electricity, sleep deprivation, and compromised melatonin production as causing a fundamental shift in the health of our heart and mitochondria. If scientists ever tackle this issue, it will be an astronomical feat for any conclusion to occur but it is an interesting thought. Until then, find ways to improve your melatonin status and improve sleep to see how you and your heart feel.
The researchers from the headline study said “Thus, the epidemic of heart failure and atherosclerosis that plagues the modern world may paradoxically be aggravated by the pervasive use of statin drugs. We propose that current statin treatment guidelines be critically reevaluated.” They were polite in their request and recommendations, but what about you? Are you going to follow the mainstream herd mentality, or are you going to look at the physiology and stand up for your health? Talk to your cardiologists and see if they understand these principles of physiology. If they did, they should be the first to stop prescribing these dangerous meds. Take charge of your health today!
 Some doctors are taking this one step further and are now laying claim to statins are also causing other forms of harm as well, pointing to an uptick in diabetes. Dr. Sachin Patel referred to a study published in 2014, Statin-associated incident diabetes: a literature review, that states that if one would review current, available clinical data that it suggests a possible association between statin use and incident diabetes in patients with underlying diabetes risk factors. Although study data may be insufficient to change the current practice paradigm, clinicians should vigilantly monitor for incident diabetes in patients on statins.
Some doctors are taking this one step further and are now laying claim to statins are also causing other forms of harm as well, pointing to an uptick in diabetes. Dr. Sachin Patel referred to a study published in 2014, Statin-associated incident diabetes: a literature review, that states that if one would review current, available clinical data that it suggests a possible association between statin use and incident diabetes in patients with underlying diabetes risk factors. Although study data may be insufficient to change the current practice paradigm, clinicians should vigilantly monitor for incident diabetes in patients on statins.
What do you think? Are statins as harmful as these two studies are suggesting?